Wouldn’t it be wonderful if we could just flip a switch and feel more calm?
While there are many tools that can help reduce stress levels, one of the most important ways to do so is by ensuring you have a well-functioning nervous system and that it maintains its impressive ability to remain plastic.
Neuroplasticity: Beyond the Brain, It’s the Whole Shebang
When we think of neuroplasticity, the flawed adage of “neurons that fire together wire together” may come to mind. Despite being simplistic and incomplete, the biggest problem with this idea is that it leads us to associate neuroplasticity exclusively with our brains.
In reality, neuroplasticity is our nervous system’s ability to adapt. This ability includes our neurons’ ability to self-repair when damaged from oxidative stress, and the prevention of cell-apoptosis, or neuron death.
But while those commonly understood characteristics of neuroplasticity are vital, the reality is that it is an incredibly complex process that refers not just to our brain, but to the entirety of our nervous system.
This fact is important and powerful because it means that we can change more than just the way our thought patterns function and our neuropathways are wired — we can alter how our entire body functions, experiences pain, and reacts to external, emotional, and interoceptive stimuli.
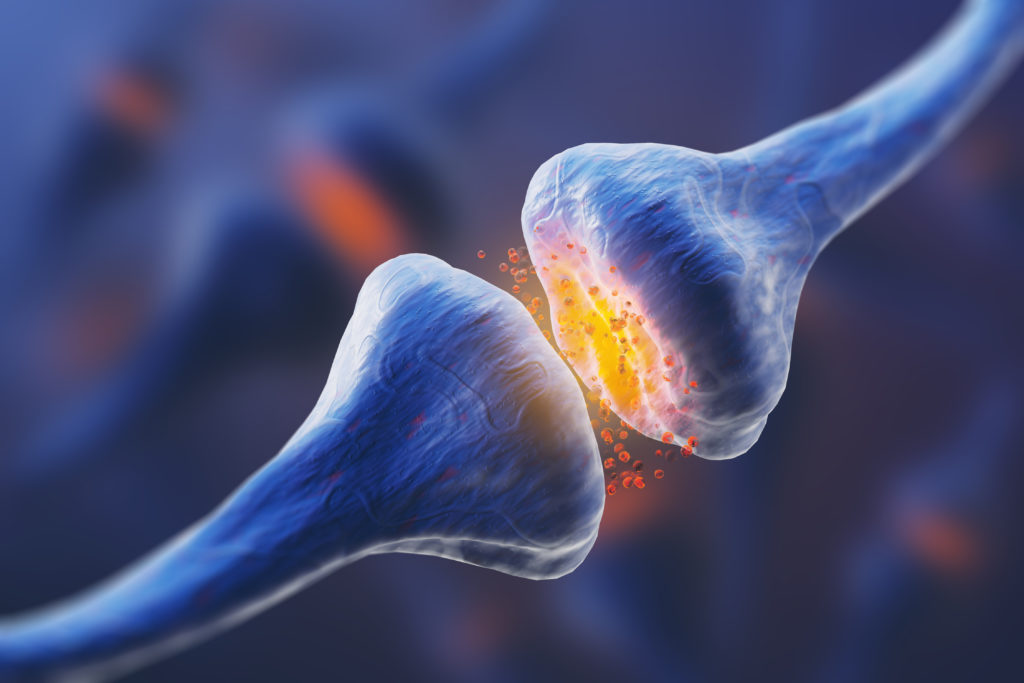
Why is it so important to include the entire nervous system in this malleable ability? As things change in our bodies and different factors impact us, it’s essential that our body and brain adapt. Without that adaptability, we would be unfit and unable to survive.
Central to this full-body adaptability is communication. And, like any good relationship, that communication must be a multi-pronged happening. This requirement is because your brain is not the only one in charge. While that may sound at odds with commonly held belief, the fact is that there are communication lines from our brain to our viscera (our organs and such) – and also from viscera to brain. (Is that where vice-versa comes from? Sorry, couldn’t help myself!)
Communication: A Multi-Splendored Thing
This bi-lateral communication happens in a few ways. Some are more subtle than others, but they include:
- Via Your Gut Neurons: Our Vagus Nerve and enteric nervous system is a whole slew of neurons embedded from our esophagus to the rectum of our GI tract that communicate efferent and afferently.
- Via Your Hormones: Your have hormones, such as leptin and ghrelin, that are produced in and along your gastrointestinal tract. These hormones cross the blood-brain barrier and send signals efferently to the brain. As such, they impact in your decisions, regulate hunger cues, and impact brain function.
- Via Your Immune Signals: Your guts are not just where the notorious growls and noises come from – it’s also the place where our immunity is rooted. Information about what we consume and the general microbe composition of our guts is passed to the brain, letting it know what we need more or less of for optimal functioning.
- Via Your Micro-metabolates: Your guts have a multitude of microbes that help us digest food and, from that process, produce short-chain fatty acids that give our brain essential information. Your enteric nervous system, – which you may have heard of being your second brain – based in your guts, creates more than 30 types of neurotransmitters, and houses 100-500 million neurons — more neurons than in your spine!
Your Essential Telephone Line
Of all of these communication pathways, the vagus nerve may be the most important. While it has gotten more attention in the mainstream media lately, you may still not have heard much about it, so if you’ll allow me a moment to geek-out, I’ll give you some background.
Etymologically speaking the vagus nerve means “the wandering nerves.” Specifically, it’s the longest of twelve nerves that starts at the top of the spine where our head meets our neck, specifically exiting from the medulla oblongata, and wriggles down our backside, touching many organs along the way, and into our guts.
But hold on, I’m sure you’re still wondering, what is it and what does it do?
As its etymological roots imply, our vagus nerve is the great wandering communicator between our organs and brain. It helps to regulate body functions like breathing, producing tears and saliva, the beating of your heart, your breath rate, sexual arousal, and other autonomic functions. More simply, you could say that its job is to keep us alive, alert and awake, breathing, and digesting along the way.
Bidirectional, Baby
As I mentioned earlier, what’s most fascinating and important is that the communication lines flow both ways along the vagus nerve, moving both from brain-to-body, which scientists call efferent communication, and body-to-brain, which they call afferent communication.
Surprisingly, the majority of vagus nerve traffic — 80% in fact — is afferent, going body-to-brain. This fact is especially surprising considering the “power” of our brain and that most of us think of it as the control center of our body.
But one of the fascinating parts of the brain is that it takes in lots of information, but only puts out new information when absolutely necessary.
Yeah, your brain is the quiet but genius type.
And because the vagus nerve is so important to this brain-to-gut-to-brain communication, we also need to be concerned with what is called “vagal tone” — basically how well the vagus nerve handles its communication responsibilities. This need for “good tone” is where malleability comes in handy — we need it to be adaptable.

When you have poor vagal tone, the communication between your gut and brain is not optimized and, as a result, the neurotransmitter, acetylcholine, (AcH for short), isn’t released.
When AcH isn’t released, it causes increased levels of inflammation throughout the body. As inflammation increases over time, it causes a whole host of physiological ramifications such as gut sensitivities and Irritable Bowel Syndrome, brain fog, autoimmune disease, anxiety, depression, and so on — all of which impede our ability to focus and sustain that focus over time.
More Vagal Tone, More Calm
All of this complexity is why many of the simplistic “tricks” to finding calm fall short. When it comes to our bodies, nothing is quite that simple. And even when simple techniques and practices prove effective, it’s important to understand what’s actually happening inside of us to cause us to improve.
Improving vagal tone is important because it helps ensure that we have wide-open lines of communication which helps our body regulate itself. But of course, it’s much more complex than that and more than we can cover in this article. The important takeaway is that the better our vagal tone, the better our neuroplasticity, which is what ultimately improves your body and brain’s ability to be less reactive under stressful situations.
In other words, we need our vagus nerve to be functioning well to be calm!
So to bring this to action here, while we clearly can do things to improve neuroplasticity, a hugely important part of feeling less stressed is also taking care to allow for optimal communication between your brain and your body, and your body and your brain, by taking care of your nervous system. This can be done in a few different, simple ways.
Ready To Give Your Vagus Nerve Some TLC?
When we are in a more parasympathetic state, we are able to create more space to engage and experience life with more empathy, but also to create space when a stressor arrives. While there are many ways to improve vagal tone (including gargling, humming, acupuncture, sighing, cold exposure, sound therapy, and brain entrainment), I’d like to focus on some of the most interesting ways to give your vagus nerve some love on a consistent basis:
| 1. Slow Deep Breathing – Focus on the exhale, or better yet, focus on the left, or non-dominant nostril to give yourself that parasympathetic activation. 2. Monitor Your HRV – Keeping our HRV elevated is a sign that our body is not stressed, and is at ease. Increasing your NEAT score, and establishing a movement practice can help prevent a low HRV. 3. Get Connected! – When we engage with others socially, and receive empathy and assurance from them, it encourages activation of our ventral nerve and parasympathetic nervous system, nurturing connection and co-regulation. 4. Supporting those microbes and micro metabolites! – Eating a diverse and colorful diet that supports your GI tract’s diversity and mobility is a crucial part of supporting your enteric nervous system! 5. Vagus Nerve Stimulation (VNS) – a small device is implanted into the left side of the chest to send electrical pulses that stimulate the brain stem. While this is certainly the most extreme of the support options, there’s incredible research being done to support its efficacy in clinical patients with epilepsy patients, to those with depression, autoimmune diseases, or even chronic pain. |
We all know the tagline, “What happens in Vegas, stays in Vegas.” While it was a bit of marketing magic for Sin City, it is the exact opposite of what happens in our bodies. In our Vagus, what happens permeates everywhere and impacts your ability to be calm and empathetic, not to mention your overall metabolic health and wellbeing.
So, should you spend time trying to be more sustainably calm? Is it worth the time, energy, and hassle? Science says, enterically speaking, absolutely.
Sources
Araujo, Laura. “Are Your Brain and Body Friends? Interoception May Be the Adhesive for Their Relationship – or the Reason Their Partnership Needs Work.” Themapsinstitute.com, 11 Oct. 2021, themapsinstitute.com/are-your-brain-and-body-friends-interoception-may-be-the-adhesive-for-their-relationship-or-the-reason-their-partnership-needs-work/. Accessed 15 June 2022.
—. “If You Ever Needed Adaptability, It’s Now. Here’s How to Use the Magic of Neuroplasticity to Teach Your Old Dog of a Brain New Tricks.” Themapsinstitute.com, 23 Apr. 2021, themapsinstitute.com/if-you-ever-needed-adaptability-its-now-heres-how-to-use-the-magic-of-neuroplasticity-to-teach-your-old-dog-of-a-brain-new-tricks/. Accessed 15 June 2022.
—. “Introduction to Meditation.” Themapsinstitute.com, 24 Aug. 2021, themapsinstitute.com/course/welcome-to-your-7-day-meditation-tour/. Accessed 15 June 2022.
—. “Nadi Shodhana: Is the Ancient Practice Just Woo – or Is It Key to Re-Balancing, and Revitalizing? For Scientists, This New Study Reveals the Unexpected.” Themapsinstitute.com, 24 Mar. 2022, themapsinstitute.com/nadi-shodhana-is-this-ancient-practice-just-woo-or-is-it-key-to-re-balancing-calming-and-revitalizing/. Accessed 15 June 2022.
—. “Why Pranayama Is the Secret Recharger You Need in Your Life.” Themapsinstitute.com, 16 Apr. 2021, themapsinstitute.com/why-pranayama-is-the-secret-recharger-you-need-in-your-life/. Accessed 15 June 2022.
Baker, Elliott, and Forshing Lui. “Neuroanatomy, Vagal Nerve Nuclei (Nucleus Vagus).” PubMed, StatPearls Publishing, 2020, www.ncbi.nlm.nih.gov/books/NBK545209/.
“Development, Diversity, and Neurogenic Capacity of Enteric Glia.” Https://Www.frontiersin.org/Article/10.3389/Fcell.2021.775102, Frontiers in Cell and Developmental Biology, 2022.
Gerritsen, Roderik J. S., and Guido P. H. Band. “Breath of Life: The Respiratory Vagal Stimulation Model of Contemplative Activity.” Frontiers in Human Neuroscience, vol. 12, 9 Oct. 2018, www.ncbi.nlm.nih.gov/pmc/articles/PMC6189422/, 10.3389/fnhum.2018.00397.
Gu, Xiaosi, et al. “Autonomic and Brain Responses Associated with Empathy Deficits in Autism Spectrum Disorder.” Human Brain Mapping, vol. 36, no. 9, 21 May 2015, pp. 3323–3338, www.ncbi.nlm.nih.gov/pmc/articles/PMC4545680/, 10.1002/hbm.22840. Accessed 15 June 2022.
Heath, Dr. Nick. “Exploring Modern Wellness.” Themapsinstitute.com, 27 Mar. 2022, themapsinstitute.com/course/breathing-for-diabetes/. Accessed 15 June 2022.
Johnson, Rhaya L, and Christopher G Wilson. “A Review of Vagus Nerve Stimulation as a Therapeutic Intervention.” Journal of Inflammation Research, vol. Volume 11, May 2018, pp. 203–213, www.ncbi.nlm.nih.gov/pmc/articles/PMC5961632/, 10.2147/jir.s163248.
Kulkarni, Subhash, et al. “Advances in Enteric Neurobiology: The “Brain” in the Gut in Health and Disease.” The Journal of Neuroscience, vol. 38, no. 44, 31 Oct. 2018, pp. 9346–9354, www.ncbi.nlm.nih.gov/pmc/articles/PMC6209840/, 10.1523/JNEUROSCI.1663-18.2018. Accessed 1 Mar. 2020.
Lycke, Nils. “IgA B Cell Responses to Gut Mucosal Antigens: Do We Know It All?” Https://Www.frontiersin.org/Article/10.3389/Fimmu.2013.00368, Frontiers in Immunology, 2013.
Mayo Clinic. “Vagus Nerve Stimulation – Mayo Clinic.” Mayoclinic.org, 2018, www.mayoclinic.org/tests-procedures/vagus-nerve-stimulation/about/pac-20384565.
“Neurons That Fire Together, Don’t Always Wire Together: Neuroscientists Uncover a New Rule of Connectivity of Neurons in the Neocortex.” ScienceDaily, www.sciencedaily.com/releases/2018/11/181108130537.htm. Accessed 15 June 2022.
“New Center to Investigate Link between Neuroplasticity and Long-Term Pain.” ScienceDaily, www.sciencedaily.com/releases/2014/10/141007092100.htm. Accessed 15 June 2022.
“The Impact of Studying Brain Plasticity.” Https://Www.frontiersin.org/Articles/10.3389/Fncel.2019.00066/Full, Frontiers in Cellular Neuroscience, 2019, www.frontiersin.org/article/10.3389/fncel.2019.00066.
The Role of Ghrelin in Regulating Synaptic Function and Plasticity of Feeding-Associated Circuits. Frontiers in Cellular Neuroscience, www.frontiersin.org/article/10.3389/fncel.2019.00205. Accessed 2019. JOURNAL=Frontiers in Cellular Neuroscience VOLUME=13 YEAR=2019 URL=https://www.frontiersin.org/article/10.3389/fncel.2019.00205.
The Role of Short-Chain Fatty Acids from Gut Microbiota in Gut-Brain Communication. Frontiers in Endocrinology, 2020, www.frontiersin.org/article/10.3389/fendo.2020.00025.
“The Vagus Nerve in the Neuro-Immune Axis: Implications in the Pathology of the Gastrointestinal Tract.” Https://Www.frontiersin.org/Article/10.3389/Fimmu.2017.01452, Frontiers in Immunology, 2017. AUTHOR=Bonaz Bruno, Sinniger Valérie, Pellissier Sonia.
TThe Vagus Nerve at the Interface of the Microbiota-Gut-Brain Axis. Frontiers in Neuroscience, 2018, www.frontiersin.org/article/10.3389/fnins.2018.00049.
Waldburger, Jean-Marc, et al. “Acetylcholine Regulation of Synoviocyte Cytokine Expression by the α7 Nicotinic Receptor.” Arthritis & Rheumatism, vol. 58, no. 11, Nov. 2008, pp. 3439–3449, 10.1002/art.23987. Accessed 7 June 2020.
Zellner, Erica. “Exploring Modern Wellness.” Themapsinstitute.com, 27 Mar. 2022, themapsinstitute.com/course/erica-zellner-ms-cns-ldn-how-stress-is-keeping-you-from-leveling-up-in-life/. Accessed 15 June 2022.
Cichon, Natalia et al. “Flavonoids as a Natural Enhancer of Neuroplasticity-An Overview of the Mechanism of Neurorestorative Action.” Antioxidants (Basel, Switzerland) vol. 9,11 1035. 23 Oct. 2020, doi:10.3390/antiox9111035.
